Cup Ear, Microtia & Anotia
Classification
There is great variety in the shape of underdeveloped ears, from a relatively minor lack of rim tissue which causes a cup deformity of the ear, through various types of microtia (micro = small, and otia = ear) to anotia (a - absent and otia = ear).
In most cases of Microtia there is a small fold of skin and cartilage at the site where the ear should be, with a small, misplaced ear lobe hanging from it.
Total anotia is rare; there is no ear structure whatsoever, and a very low hairline.
CUP EAR
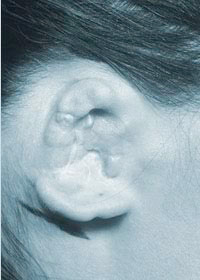
A cup ear is usually cup-shaped and very difficult to push back into a normal position against the side of the head, because there is too little tissue in the rim. It is sometimes called a constricted ear, because the outer border of the ear, the rim, constricts the edge of the ear and prevents it from lying flat.
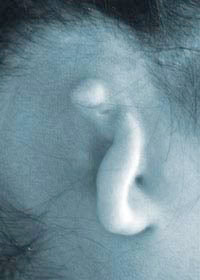
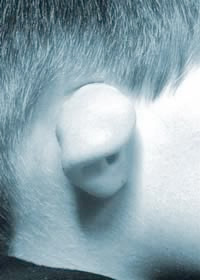 A severely cupped ear before surgery
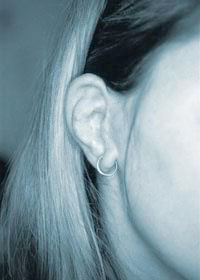
A severely cupped ear before surgery 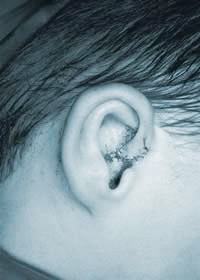 Cup ear 10 days after surgery, stitches present
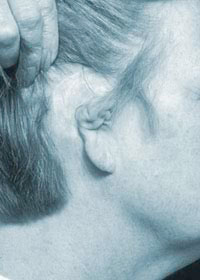
Cup ear 10 days after surgery, stitches present 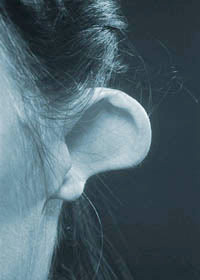 A cupped upper pole and absent lower pole pre-op
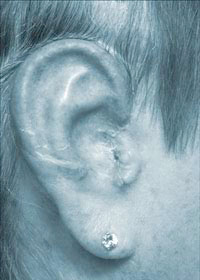
A cupped upper pole and absent lower pole pre-op 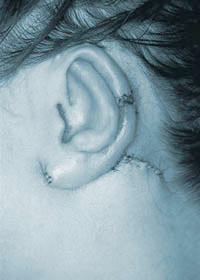 The reconstructed ear immediately after surgery
The reconstructed ear immediately after surgery Microtia and Anotia
Microtia & Anotia affect about 1 in 6000 children worldwide. The figures are higher in some populations (estimated at 1 in 4,000 in the Japanese, and as high as one in 1 in 1200 births in Navajo Indians). It is generally stated that there are four grades of microtia, although the grading system means little in practice. Grade I is the mildest form; the ear has a normal shape but is smaller than usual. Anotia, the total absence of any ear elements is considered to be Grade IV.
conchal microtia
In Conchal Microtia, a good part of the upper ear is developed but abnormally folded. Conchal microtia is generally called Grade II microtia.
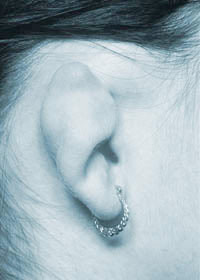 Conchal microtia before reconstruction
Conchal microtia before reconstruction 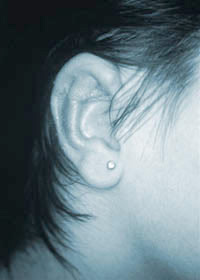 Conchal microtia after reconstruction
Conchal microtia after reconstruction Grade III Microtia
Grade III is the most common form of microtia, with variable amounts of ear tissue present.
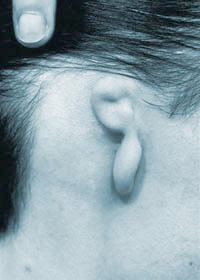 Before Surgery
Before Surgery 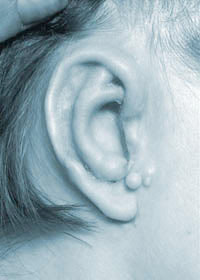 After the first stage of surgery
After the first stage of surgery The right side is more commonly affected than the left, and males are more often affected than females. In one in ten cases, both a baby's ears will be affected.
 Before surgery
Before surgery 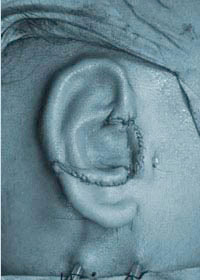 Immediately after the first stage of surgery, drains in place
Immediately after the first stage of surgery, drains in place Polyotia or Mirror Ear
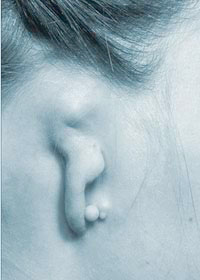
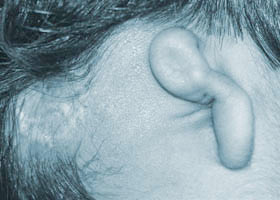
Rarely, persistent pre-auricular tissues are so large that they resemble an extra ear and the term polyotia is used. The “second” ear can appear as a mirror image folded forward and lying on the posterior cheek, and the term mirror ear is also applied.
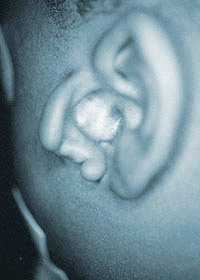
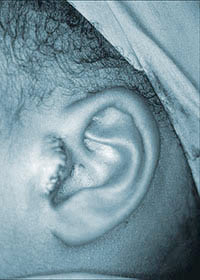
TWO REMNANT MICROTIA AND ANOTIA
In a small number of patients, a narrow strip of normal skin separates two small ear remnants (two remnant Microtia) and there is usually facial nerve weakness on the affected side.
In anotia, there is no ear tissue whatsoever.
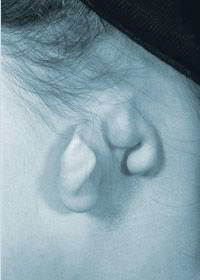 Two-remnant microtia deformity
Two-remnant microtia deformity 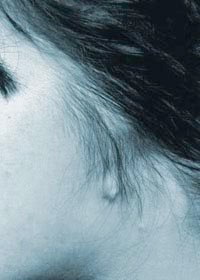 Anotia - the lack of an ear from birth
Anotia - the lack of an ear from birth Embryology
A primitive ear shape is recognizable in a 50 day old embryo. The ear forms initially in the neck region and moves upwards onto the head by week 10. In many birth abnormalities involving the ear, this migration is disturbed and the ear remains low-set.
The problem that results in Microtia occurs in the womb about 7-8 weeks after the baby is conceived. The most likely cause is an interruption of the blood supply to the area which will form the ear. Microtia & Anotia are sometimes seen as isolated problems or sometimes as part of a syndrome such as Goldenhar syndrome, hemifacial microsomia or Treacher Collins syndrome.
Surgery
Treatment for Microtia & Anotia is not necessarily essential, and some patients do not wish to have the defect reconstructed. For those who want the defect corrected, there are two reconstructive options: to have the ear rebuilt from their own tissue (autogenous ear reconstruction), or to have a prosthetic or false ear anchored to the bone on the side of the head by titanium fixtures (a bone-anchored prosthesis). Patients with Anotia usually also require lobe reconstruction.
The gold standard of ear reconstruction is an ear of carved autogenous costal cartilage, and almost all patients prefer this technique, since the aesthetic results are now very good. It is usually possible to mimic the opposite normal ear in shape and size. Results have improved enormously in recent years.
The ideal age for surgery is over the age of 10 or when the chest circumference is over 60 centimetres, so that the ribcage has grown enough to allow enough cartilage to be harvested. Surgery earlier than 10 years is possible if the patient is being teased, or if there are other pressures to have the reconstruction carried out a little earlier. It is very common for surgery to be undertaken in the summer holidays before a child moves from primary to secondary school.
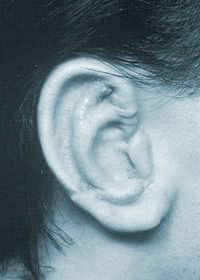
When to have microtia surgery
The ideal age for surgery is over the age of 10 or when the chest circumference is over 60 centimetres, so that the ribcage has grown enough to allow enough cartilage to be harvested. Surgery earlier than 10 years is possible if the patient is being teased, or if there are other pressures to have the reconstruction carried out a little earlier. It is very common for surgery to be undertaken in the summer holidays before a child moves from primary to secondary school.
Some microtia patients are confident enough about their "little ear" to decline surgery until they are adults. There is no upper age limit to autogenous ear reconstruction, although the likelihood that the cartilage might calcify and become harder to carve (like bone) increases slightly with age. If a bone-anchored prosthesis is to be used then the bone at the ear site needs to be of adequate thickness to accept the fixtures.
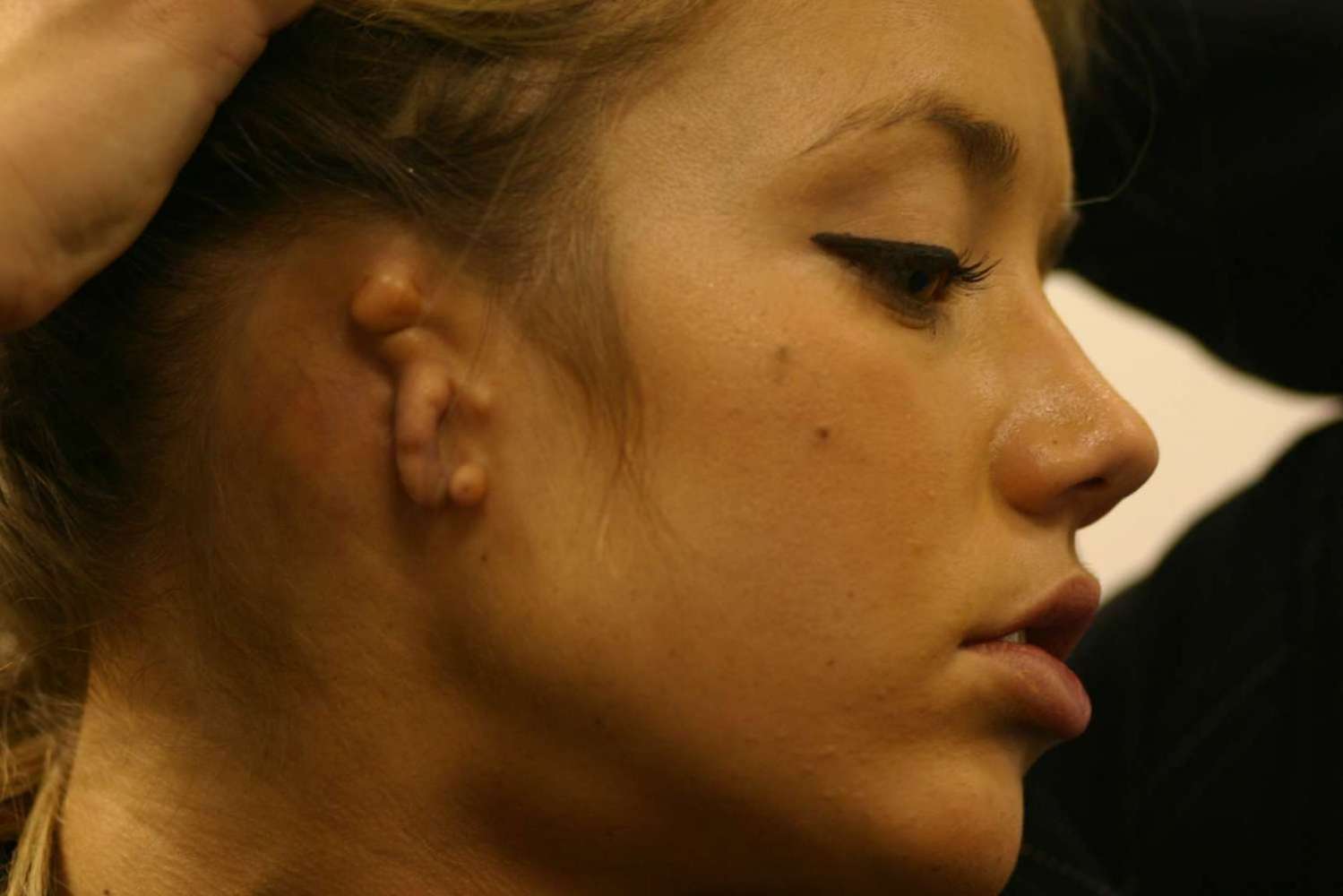 Actor and model Sasha Gardner
Actor and model Sasha Gardner 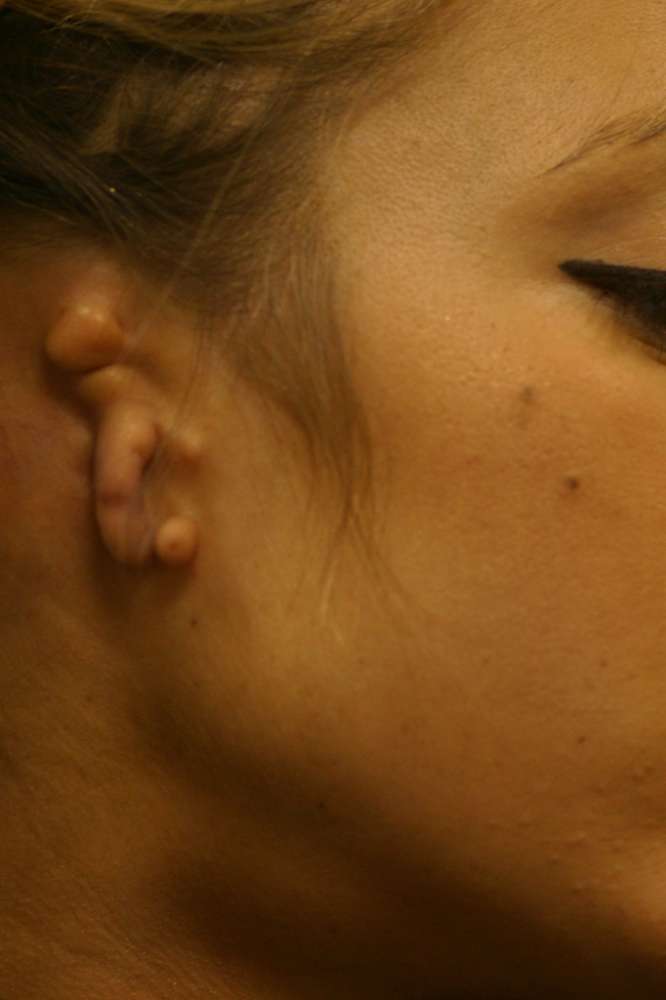 Close-up before surgery
Close-up before surgery  After surgery
After surgery Hearing and microtia
There is usually hearing loss on the affected side as the middle ear is underdeveloped. If only one side is affected, then a hearing aid is not normally needed. When the condition affects both sides, treatment to improve the hearing is important. If bone-anchored hearing aids are to be used, it is very important that the aids are properly positioned so as not to compromise the tissues for autogenous ear reconstruction.
 Microtia patient with scarring from a BAHA
Microtia patient with scarring from a BAHA 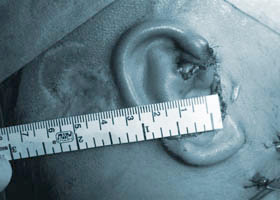 Immediately post-op, showing how much space is required for the new ear
Immediately post-op, showing how much space is required for the new ear Fixing failed ear reconstruction
Autogenous reconstruction for Microtia is best carried out on previously un-operated sites. Earlier surgery can remove valuable skin and causes scars which can interfere with the blood supply to the new ear. Without realising that they are compromising the final result, it is not uncommon for well-meaning surgeons to perform interim “tidy up” procedures, such as lobe or lop ear set-back, in an attempt to improve the appearance of the ear site until the child is old enough for a formal reconstruction. All such attempts make definitive surgery more difficult, at best, and at worse they spoil the final result and should be strongly resisted.
Books
Gault DT
Total Reconstruction of the Pinna - a chapter for Scott Brown's Otorhinolaryngology, Head and Neck Surgery, 7th Edition Arnold
Gault DT and Rothera M
Management of Congenital Deformities of the External and Middle Ear - a chapter for Scott Brown's Otorhinolaryngology, Head and Neck Surgery, 7th Edition Arnold
Gault DT
Reconstruction of the ear - a chapter for Principles and Practice of Head and Neck Oncology
Editors Peter Rhys Evans, Patrick Gullane & Paul Montgomery. Martin Dunitz 2003 Winner for George Davey Howells Memorial Prize for most distinguished published contribution to the advancement of Otolaryngology during the preceding five years.
Relevant publications
Chana JS, Grobbelaar AO & Gault DT. (1997)
Tissue expansion as an adjunct to reconstruction of congenital and acquired auricular deformities.
British Journal of Plastic Surgery 50:456-462
Harris P, Ladhani K, Das Gupta R and Gault DT. (1999)
Reconstruction of Acquired Subtotal Ear Defects with Autogenous Costal Cartilage.
British Journal of Plastic Surgery 52: 268-275.
Gault DT. (1998)
Ear Reconstruction : Pitfalls and Tips
Face 6: 15-16
Sabbagh W, Withey S and Gault DT (1999)
A simple alternative to ear reconstruction (letter)
British Journal of Plastic Surgery 52:80-81.
Chana JS, Grobbelaar AO and Gault DT (1998)
Tissue expansion: a useful adjunct to auricular reconstruction
Face 6: 65-68.
Gault D. (1999)
Reconstruction for microtia.
Journal of Laryngology and Otology Supplement no 23. Vol 113, page 27.
Botma M, Aymat A, Gault D, Albert D
Rib graft reconstruction vs Osseointegrated prosthesis for microtia: A significant change in patient preference.
Clinical Otolaryngology. 2001, 26, 274-277
Lawson K, Waterhouse N, Gault DT, Calvert ML, Botma M, Ng T.
Is hemifacial microsomia linked to multiple maternities?
British Journal of Plastic Surgery 2002 55, 474-478
Sabbagh W and Gault D
Location, location, location
Journal of Laryngology and Otology; 2004 118: 738-740
Bajaj Y, Wyatt M, Gault D, Bailey M, Albert DM
How we do it: BAHA positioning in patients with microtia requiring auricular reconstruction
Clinical Otolaryngology 2005 30: 468-471.
Horlock N, Vogelin E, Bradbury ET, Grobbelaar AO, Gault DT
Psychosocial outcome of patients after ear reconstruction - a retrospective study of 62 patients.
Annals of Plastic Surgery 54: (5): 517-524 2005
Vadodaria S, Mowatt D , Giblin V, Gault D
Mastering ear cartilage sculpture: the vegetarian option
Plastic and Reconstructive Surgery 116(7), Dec 2005 2043-2044 Annals of Plastic Surgery 54: (5): 517-524 2005
Gore S, Myers S, Gault D
Mirror ear: a reconstructive technique for substantial tragal anomalies or polyotia
Journal of Plastic, Reconstructive and Aesthetic Surgery 59, 499-504 2006
Beckett KS and Gault D
Operating in an eczematous surgical field; Don't be rash, delay surgery to avoid infective complications
Accepted by the British Journal of Plastic Surgery 2006
